Contents
- 1 What is Genital Herpes?
- 2 Genital Herpes Pictures
- 3 Causes of Genital Herpes
- 4 Ways of Genital Herpes Transmission
- 5 Forms and Manifestations of Genital Herpes
- 6 Genital Herpes and Pregnancy
- 7 Genital Herpes in Newborns
- 8 Diagnosis of Genital Herpes
- 9 Treatment of Genital Herpes
- 10 Medicines for the Treatment of Genital Herpes
- 11 List of Genital Herpes Medications
- 12 Prevention and Prophylaxis
What is Genital Herpes?
Genital herpes is a sexually transmitted disease caused by the herpes simplex virus (HSV), and causes herpetic sores on the genitals.

Genital herpes is a viral lesion of the genital mucosa, characterized by the appearance of blisters, followed by erosions and sores. It is accompanied by a local burning sensation, swelling, hyperemia, an increase in inguinal lymph nodes and signs of intoxication. It causes relapses and can subsequently lead to serious complications: reduction of local and general immunity, development of bacterial infections of the genitals, damage to the nervous system, development of cervical and prostate cancer. It is especially dangerous in pregnant women, because it increases the likelihood of spontaneous miscarriage, pathology and even death of a newborn. It is included in the group of sexually transmitted diseases (STDs).
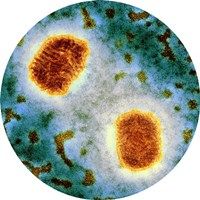
 The causative agent of genital herpes is the herpes simplex virus (HSV). About 90 percent of people have this STD.
The causative agent of genital herpes is the herpes simplex virus (HSV). About 90 percent of people have this STD.
There are several types of herpes virus causing skin, mucous membrane, central nervous system and other organs (herpes simplex virus types 1 and 2, cytomegalovirus, varicella, Epstein-Barr virus, shingles, etc.). Herpes simplex virus causes oral and genital forms of the disease. The 1 type of HSV affects mainly the face, lips, wings of the nose, the 2 type of HSV in most cases causes the genital herpes. HSV is often detected in collaboration with ureaplasma and cytomegalovirus.
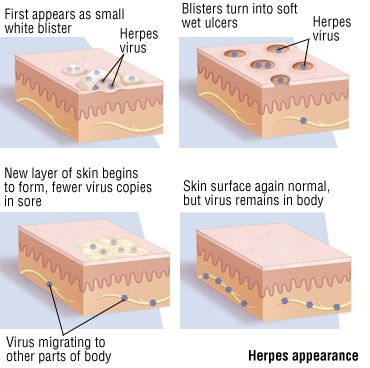 Genital herpes has a sexual way of transmission, with various forms of sexual contacts it easily penetrates through the damaged skin and the epithelium of the mucous membrane. After infection, HSV migrates to the nerve ganglia, remaining there for lifetime. Propagation of HSV in epithelial cells of the skin and mucous membranes leads to their dystrophy and death. Infection is characterized by a chronic course and manifests cyclically: periods of activity or relapse (2-21 days), accompanied by the appearance of sores in the form of blisters (fluid-filled bumps), alternate with periods of remission, when clinical symptoms disappear. In most cases the genital herpes is asymptomatic, but patients still remain the main source of infection.
Genital herpes has a sexual way of transmission, with various forms of sexual contacts it easily penetrates through the damaged skin and the epithelium of the mucous membrane. After infection, HSV migrates to the nerve ganglia, remaining there for lifetime. Propagation of HSV in epithelial cells of the skin and mucous membranes leads to their dystrophy and death. Infection is characterized by a chronic course and manifests cyclically: periods of activity or relapse (2-21 days), accompanied by the appearance of sores in the form of blisters (fluid-filled bumps), alternate with periods of remission, when clinical symptoms disappear. In most cases the genital herpes is asymptomatic, but patients still remain the main source of infection.
Genital Herpes Pictures
Causes of Genital Herpes
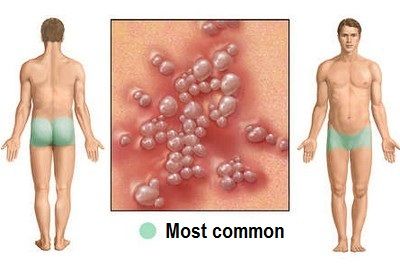 Primary infection of HSV is usually airborne in childhood (the incidence rate is 50 % in the age of 6-7 years). The reasons are the high population density, low socioeconomic standards of living, non-compliance with hygiene rules.
Primary infection of HSV is usually airborne in childhood (the incidence rate is 50 % in the age of 6-7 years). The reasons are the high population density, low socioeconomic standards of living, non-compliance with hygiene rules.
Secondary infection occurs, as a rule, as a result of sexual contacts. A high incidence of genital herpes is observed among people of 20-30 years old. This is due to the early sexual activity, promiscuous sexual intercourse, frequent changes of partners, unprotected sex. Other risk factors of genital herpes are the following:
- decreased immune defenses;
- the presence of STDs;
- the sex of a person (it is noticed that women suffer from genital herpes more often than men);
- surgical termination of pregnancy, use of intrauterine spirals.
The human immune system responds to the penetration of HSV by the production of specific antibodies, clinical manifestations of infection are not observed at normal levels of immune responses. Under the influence of unfavorable factors that reduce the immune reactivity of the body, HSV is activated, which is manifested by sores on the skin and mucous membranes, neuralgic pains. Episodes of recurrences of genital herpes often appear because of chronic stress, lack of vitamins, hypothermia, overheating, climate change.
Ways of Genital Herpes Transmission
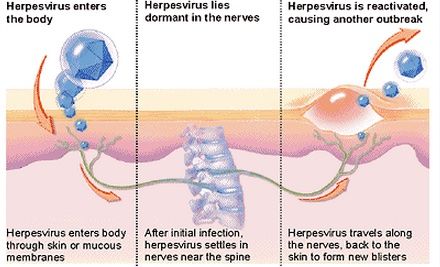 Infection with genital herpes often occurs through the mucous membranes of the genital organs, rectum, urethra or skin damage during genital, oral - genital or anal - genital contacts.
Infection with genital herpes often occurs through the mucous membranes of the genital organs, rectum, urethra or skin damage during genital, oral - genital or anal - genital contacts.
Transmission of HSV is also possible:
- through airborne droplets;
- from the infected mother to the fetus (during a contact with the mother's birth canal, transplacentally, from the external genital organs through the cervical canal into the uterine cavity);
- self-infection - autoinoculation (the infected person transfers the infection from infected areas of the body to the uninfected ones);
- by household means - rarely (through items of hygiene).
The infection with genital herpes typically occurs when the infected partner does not even know about the disease, since it has no clinical manifestations of the disease (in the case of asymptomatic virus).
Forms and Manifestations of Genital Herpes
The clinical course distinguishes primary genital herpes (the first episode of the disease) and recurrent (all subsequent episodes of the disease).
Recurrent genital herpes can occur in typical, atypical clinical forms and in the form of asymptomatic virus.
Primary Genital Herpes
The earliest symptoms of primary genital herpes include swelling, redness, pain, burning sensation. Local manifestations of genital herpes are often accompanied by a rise in temperature, malaise, headache and muscle pain. After a few days, there are herpetic eruptions - small fluid-filled blisters. The rupture of blisters is accompanied by the formation of painful erosive-ulcerative elements. With the localization of sores on the genitals, painful urination is noted.
The genital herpes in women usually affects the external genitalia, crotch and anus, urethra, inner thighs. In men, herpetic eruptions on genitals are most often localized on foreskin of the penis, less often in the urethra, sometimes accompanied by the development of herpetic urethritis or prostatitis.
Recurrent Genital Herpes
The development of recurrences of genital herpes occurs in 50-70% of cases in patients who underwent a primary infection. Depending on the frequency of repeated episodes, several forms of recurrent genital herpes are distinguished:
- light form (relapses occur not more than 3 times a year)
- medium-heavy form (from 4 to 6 times a year)
- severe form (monthly relapses)
The course of recurrent genital herpes can be arrhythmic, monotonous and subsiding.
The arrhythmic course of genital herpes is characterized by alternating remissions from 2 weeks to 5 months. In this case, the long periods of remission can cause intense and prolonged relapses of genital herpes.
During the monotonous course of genital herpes, frequent episodes of the disease are observed after slightly changing periods of remission. This type includes menstrual herpes, which has a persistent current and is difficult to treat.
A more favorable course has the genital herpes of subsiding type. It is characterized by a decrease in the intensity of relapses and an increase in the periods of remission.
The development of recurrences of genital herpes occurs under the influence of various factors: hypothermia, sexual intercourse, stressful situations, overfatigue, the emergence of another pathology (influenza, ARVI).
Symptomatically, the relapses of genital herpes are weaker than the primary disease; however, their consequences can be much more serious.
Herpetic eruptions are accompanied by extreme soreness, making it difficult for the patient to move, to visit the toilet, disturbing their sleep. Quite often the psychological state of a person changes: there is irritability, fear of new rashes, fear for the health of relatives, suicidal thoughts, etc.
Atypical Forms of Genital Herpes
Atypical forms of genital herpes are erased, in the form of chronic inflammation of the external and internal genital organs (vulvovaginitis, colpitis, endocervicitis, urethritis, cystitis, prostatitis, etc.). The diagnosis of genital herpes is based on laboratory confirmation of the herpetic infection presence. Atypical forms of genital herpes are more than half of the clinical cases - 65%.
An atypical form of genital herpes is characterized by mild puffiness, areas of erythema, small blusters, persistent burning and itching; abundant, not amenable to therapy leucorrhoea. During the prolonged course of genital herpes, there is an increase and soreness of the inguinal lymph nodes.
According to the localization of herpetic eruptions, three stages are distinguished:
- I stage - genital herpes affects the external genitalia;
- II stage - genital herpes affects the vagina, cervix, urethra;
- III stage - genital herpes affects the uterus, epididymis, bladder, prostate.
The advanced stage of genital herpes can lead to immunodeficiency; the risk of infertility and cervical cancer in women. HSV is dangerous for people with weakened immunity (HIV-infected) and for patients undergone an organ transplant operation.
Genital Herpes and Pregnancy
 The greatest danger during pregnancy is primary infection of genital herpes, if there were no manifestations of the disease previously. If the infection occurred early in pregnancy there is a possibility of malformation, when the organs and tissues are growing in fetus. HSV can be transmitted through the placenta, affecting mainly the neural tissue of the fetus. Genital herpes increases the threat of spontaneous miscarriage, premature birth, fetal deformities and death.
The greatest danger during pregnancy is primary infection of genital herpes, if there were no manifestations of the disease previously. If the infection occurred early in pregnancy there is a possibility of malformation, when the organs and tissues are growing in fetus. HSV can be transmitted through the placenta, affecting mainly the neural tissue of the fetus. Genital herpes increases the threat of spontaneous miscarriage, premature birth, fetal deformities and death.
Pregnant women with atypical forms of genital herpes in the last 6 weeks of pregnancy should be tested twice for HSV. When a herpes virus is detected, the cesarean section is performed to avoid possible infection of the fetus when passing through the birth canal.
The best option is to screen women for HSV during the pregnancy preparation, as well as during the pregnancy.
Genital Herpes in Newborns
In most cases, the fetal infection occurs in the first 4-6 hours during childbirth as the child passes through the mother's infected birth canal. Usually, HSV in newborns enter the eyes, mucous membranes of the mouth, skin, respiratory tract. After primary infection of a newborn, HSV is spreading in the body by hematogenous or contact ways. The probability of newborns’ infection increases with the infection of a mother in the last trimester of pregnancy.
 With the localized form of herpetic infection, redness, vesicles, hemorrhages of the skin and mucous membrane of the mouth can develop in the newborn, as well as meningoencephalitis, keratoconjunctivitis, chorioretinitis (inflammation of the blood vessels and retina) and lens-form opacity. Children infected with genital herpes suffer from persistent neurological disorders.
With the localized form of herpetic infection, redness, vesicles, hemorrhages of the skin and mucous membrane of the mouth can develop in the newborn, as well as meningoencephalitis, keratoconjunctivitis, chorioretinitis (inflammation of the blood vessels and retina) and lens-form opacity. Children infected with genital herpes suffer from persistent neurological disorders.
Genital herpes can cause the development of generalized infection of newborns. Signs of generalized herpetic infection appear after 1-2 weeks. Local symptoms include aversion to food, vomiting, fever, jaundice, respiratory distress, bleeding, shock. The death of a child can come from blood loss and vascular insufficiency.
Diagnosis of Genital Herpes
 In case of the genital herpes diagnosis, the venereologist takes into account all the complaints, history and objective research. Diagnosis of typical cases of genital herpes, as a rule, is not complicated and is based on clinical manifestations. Herpetic sores that exist for a long time should be distinguished from syphilitic sores.
In case of the genital herpes diagnosis, the venereologist takes into account all the complaints, history and objective research. Diagnosis of typical cases of genital herpes, as a rule, is not complicated and is based on clinical manifestations. Herpetic sores that exist for a long time should be distinguished from syphilitic sores.
Laboratory methods for diagnosing genital herpes include:
- methods for detecting HSV on the material of the affected organs (scrapings from the vagina and cervix, smear from the urethra, histological material of the fallopian tubes, etc.). The method of growing HSV on tissue culture and subsequent study of its properties is applied; the method of virus recognition under the electron microscope is used;
- Methods for detecting antibodies to HSV in the blood serum (immunoglobulins M and G). They can detect genital herpes even in asymptomatic conditions and identify antibodies to HSV of 1 or 2 types. These include ELISA - the method of immuno-enzyme analysis.
Treatment of Genital Herpes
 Existing HSV drugs can reduce the course of genital herpes, but not able to eliminate the disease completely.
Existing HSV drugs can reduce the course of genital herpes, but not able to eliminate the disease completely.
In order to avoid the development of HSV resistance to classical antiviral drugs (acyclic nucleosides - Valaciclovir, Acyclovir, Famciclovir), they are recommended to be used alternately, as well as in combination with interferon. Interferon has a powerful antiviral effect, and its deficiency is one of the main causes of genital herpes recurrence.
There are different ready-made medicines in the form of ointments, containing acyclovir and interferon, which usually contain lidocaine, providing a local anesthetic effect, which is extremely important in the case of painful manifestations of genital herpes. The use of such combination of drugs in patients with genital herpes provides the sores healing on the 5th day of treatment.
Medicines for the Treatment of Genital Herpes

The main drugs that are commonly used to treat the symptoms of genital herpes are acyclovir (Zovirax), famciclovir (Famvir) and valaciclovir (Valtrex). All of them are produced in the form of pills, and they are highly effective. Special severe cases can be treated with intravenous acyclovir in a hospital.
List of Genital Herpes Medications
| Medications to treat Genital Herpes |
| acyclovir |
| Zovirax |
| Abreva |
| Blistex |
| docosanol |
Prevention and Prophylaxis

The method of preventing the primary genital herpes infection is the use of condoms for casual sexual intercourse. However, even in this case, the probability of HSV infection through microcracks and damage to mucous membranes and skin not covered by a condom remains high. It is possible to use local antiseptic drugs to treat areas, which may be exposed by a virus.
The recurring course of genital herpes is observed with a decrease in the body's defenses: diseases, overheating, hypothermia, menstruation, pregnancy, hormonal drugs, stress. To prevent the genital herpes recurrence, it is important to have a healthy lifestyle, adequate nutrition and rest, take vitamins. The measures of genital herpes’ preventing include: personal hygiene activities, the prompt identification and treatment of sexually transmitted diseases.
A patient infected with HSV should warn their partner about the symptoms. Since there is a possibility of infection during sexual intercourse in case of the absence of herpetic eruptions, the use of a condom is also necessary.
After an unprotected sexual contact, it is possible to resort to the method of emergency prophylaxis of genital herpes with a locally active antiviral drug in the first 1-2 hours after sexual intercourse.
For the prevention of self-infection, when the genital herpes virus is transferred with dirty hands from the lips to the genitals, it is necessary to perform basic hygienic requirements: careful and frequent hands washing (especially if there is fever on the lips); use of individual towels for hands, face and body.
In order to reduce the risk of HSV infection in newborns, pregnant women with genital herpes need to undergo the operative delivery (caesarean section). In case of planned natural births, women with a recurrent course of genital herpes are prescribed a preventive course of aciclovir.
After the unprotected sex, during the pregnancy and in case of sexual relations with the carrier of HSV, it is recommended to be screened for genital herpes and other STDs.