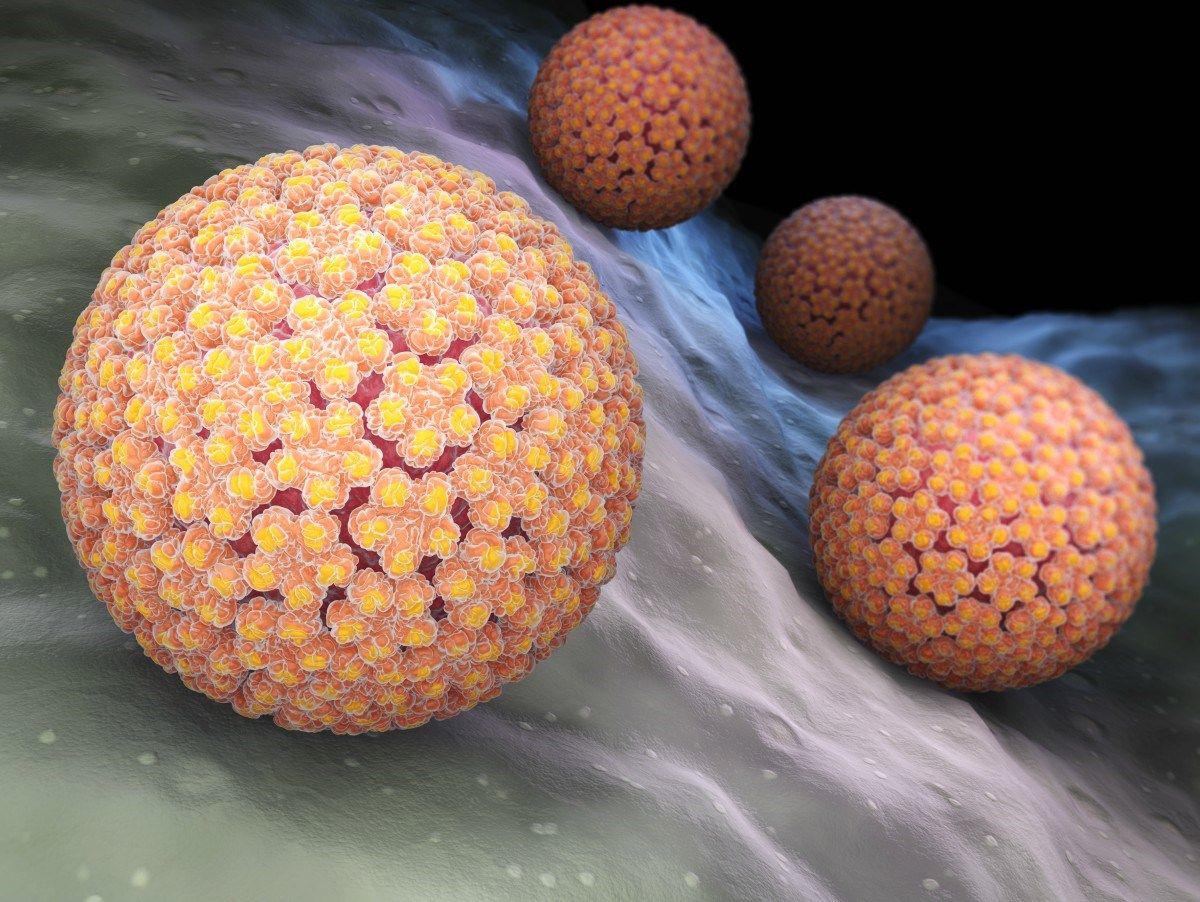
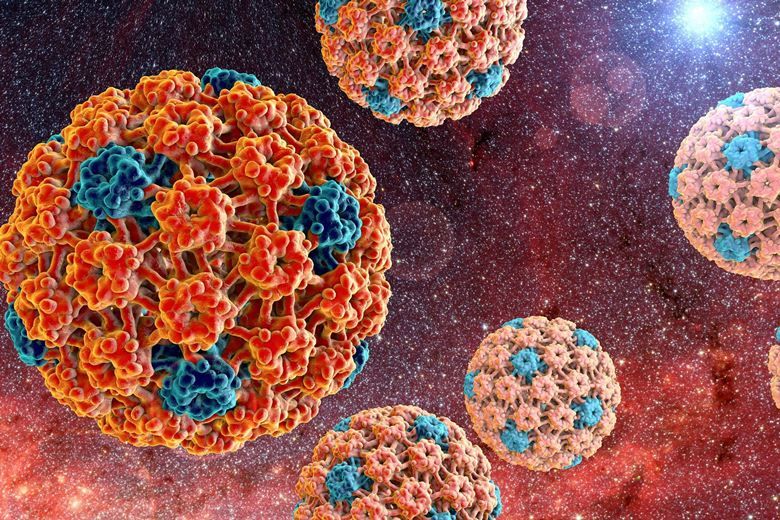
Human papillomavirus is the most common sexually transmitted disease. Because HPV is so widespread, it's important for anyone who is sexually active to understand the disease's causes, symptoms, and treatments.
 |
 |
What Is Human Papillomavirus (HPV) / Genital Warts?
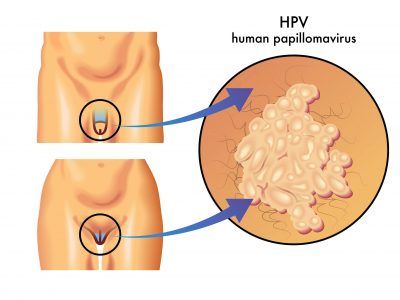
HPV is a sexually transmitted infection that is passed from person to person through skin contact. Most sexually active people become infected at some point in their lives, and some people are repeatedly infected.
There are many varieties of HPV, and different varieties lead to different symptoms and complications. Some strains of HPV cause warts, and others cause more serious health issues like cancer. Although there is no cure, most symptoms can be treated or will resolve on their own.
How Do You Get HPV / Genital Warts?
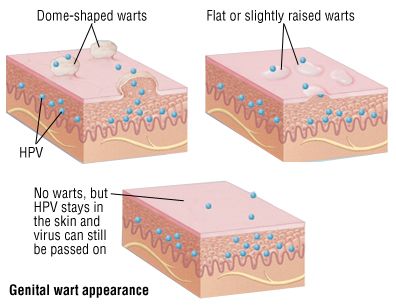 HPV spreads through skin contact with the genitals, so having sexual intercourse with someone who is infected puts you at risk of contracting the virus. The disease can affect anyone who is sexually active, but it often remains dormant and causes no symptoms. However, even if you have no signs or symptoms, you can still pass the disease to someone else.
HPV spreads through skin contact with the genitals, so having sexual intercourse with someone who is infected puts you at risk of contracting the virus. The disease can affect anyone who is sexually active, but it often remains dormant and causes no symptoms. However, even if you have no signs or symptoms, you can still pass the disease to someone else.
In some cases, symptoms don't develop until years after sexual contact with an infected person. Therefore, it can be difficult to determine when you were first infected. The virus can also be transmitted to an infant during birth.
HPV Pictures
Risk Factors
Anyone who is sexually active can contract HPV, but some people are at a greater risk than others. The following are some of the biggest risk factors for contracting HPV or developing complications from the disease:
- Weakened immune system
- Having areas of damaged skin
- Having a large number of sexual partners
- Having sex with someone with multiple sexual partners
- Using tobacco
Facts
 Here are some fast facts about HPV:
Here are some fast facts about HPV:
- There are over 100 varieties of HPV.
- About 80 percent of sexually active people have HPV, but most are unaware.
- Around 79 million Americans currently have HPV.
- HPV can be spread through vaginal, oral, and anal sex regardless of whether or not an infected person has any symptoms.
- Some strains of HPV can lead to cancer, but there is no way of knowing which infected people will develop cancer.
- Every year, 12,000 women in the U.S. are diagnosed with cervical cancer, the cancer most commonly associated with HPV.
Signs and Symptoms
Most people who contract HPV won't experience any symptoms or health issues. In many cases where symptoms do appear, they will clear up without requiring medical treatment.
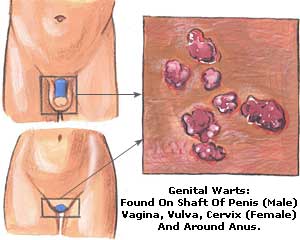 Some low-risk types of HPV cause genital warts, which are soft, fleshy bumps that often appear in small clusters. They typically affect the vulva and cervix in women and the penis and scrotum in men. Genital warts are usually painless and can easily be treated or removed. HPV can also cause common warts, plantar warts, and flat warts.
Some low-risk types of HPV cause genital warts, which are soft, fleshy bumps that often appear in small clusters. They typically affect the vulva and cervix in women and the penis and scrotum in men. Genital warts are usually painless and can easily be treated or removed. HPV can also cause common warts, plantar warts, and flat warts.
Unfortunately, high-risk types of HPV that can lead to cancer or other serious health problems often don't cause any symptoms until the damage is done. Regular checkups are essential for detecting HPV early and preventing complications. Symptoms of cervical cancer, one of the most common cancers associated with HPV, include the following:
- Vaginal bleeding between periods or after sexual intercourse
- Fatigue
- Loss of appetite
- Back, leg, or pelvic pain
- Vaginal pain or discomfort
Causes
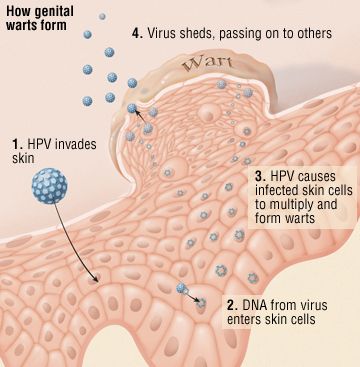
HPV is caused by a virus that spreads with skin-to-skin contact. There are over 100 types of HPV, and more than 30 of them can affect the genitals. Some strains rarely cause symptoms, some cause warts, and some can cause cervical cancer and other forms of cancer.
Types 6 and 11 are usually responsible for genital warts, but they're considered low-risk varieties of HPV. About a dozen varieties of HPV can lead to cancer, but types 16 and 18 cause most HPV-related cancer cases.

Testing and Diagnosis
In 2014, the FDA approved the first HPV DNA test. The test detects the high-risk forms of HPV, and it's usually done in conjunction with a Pap smear. The CDC recommends that women have their first Pap smear and HPV test at the age of 21 and repeat both tests every three years. Then, from the ages of 30 to 65, women should be tested every five years.

In some cases, doctors may diagnose HPV based on a Pap smear alone. Although Pap smears don't detect HPV, they can detect cell changes that are typically caused by HPV. However, if your Pap smear does show abnormal cell changes, your doctor will probably recommend an HPV test to diagnose the disease with certainty.
You shouldn't panic if your HPV test has positive results. It doesn't mean that you have cancer or that you will definitely develop cancer. If the test indicates that you have one of the HPV strains that can cause cancer, your doctor may recommend more frequent checkups or Pap smears to look for cervical changes. If something abnormal appears, you may need to undergo a cervical biopsy to check for cancer.
There isn't a test that can diagnose HPV in men. In most cases, doctors will diagnose the disease in men with a visual inspection.
Prevention
The best way to prevent HPV is to avoid sexual contact with others. Most people become sexually active at some point in their lives, though, and there are other ways to reduce your risk of contracting the disease. Practicing safe sex by using condoms and dental dams can help you prevent HPV, and being in a monogamous sexual relationship will reduce your risk as well.
Regular checkups, Pap smears, and HPV tests may not prevent you from contracting the disease, but they can prevent you from passing it to a sexual partner. If you discover that you have HPV, you can take the necessary precautions to avoid spreading it.
Getting the HPV vaccine is one of the most foolproof ways to prevent HPV, especially the high-risk strains that can cause cancer. Anyone between the ages of nine and 26 can be vaccinated.
Treatment
HPV doesn't have a cure, but 70 to 90 percent of cases are cleared up by the immune system without treatment. When treatment is necessary, the goal is usually to relieve or manage the symptoms of the disease.
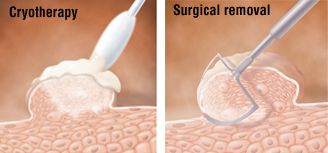 There are several options for removing warts and abnormal cells. One popular treatment is cryosurgery, which involves using liquid nitrogen to freeze off the warts. Electrocautery is a procedure that burns off the warts with an electrical current, and laser therapy destroys the warts with an intense light. You could also have a loop electrosurgical excision procedure, or LEEP, which involves using a wire loop to remove abnormal cells.
There are several options for removing warts and abnormal cells. One popular treatment is cryosurgery, which involves using liquid nitrogen to freeze off the warts. Electrocautery is a procedure that burns off the warts with an electrical current, and laser therapy destroys the warts with an intense light. You could also have a loop electrosurgical excision procedure, or LEEP, which involves using a wire loop to remove abnormal cells.
Your doctor may also prescribe medications like podophyllin, imiquimod, or podofilox to remove the warts. Common warts can be treated with over-the-counter medicines, but you shouldn't apply over-the-counter products to genital warts.
It's important to remember that removing warts does not eliminate the virus from your body. Unfortunately, there isn't a treatment that will remove the virus (just like the herpes virus).
HPV and Cancer
HPV types 16 and 18 cause about 70 percent of cervical cancer cases. HPV is also linked to other genital cancers and throat cancers. Not all strains of HPV can cause cancer, but cervical cancer is the most common HPV-related disease.
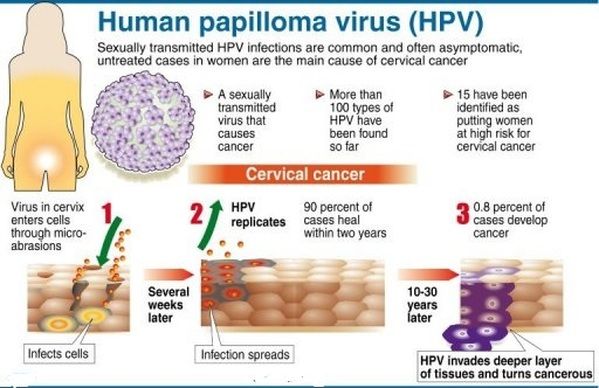
Cancer often doesn't develop until many years after an HPV infection. If you have a normal immune system, it can take 15 to 20 years for cervical cancer to develop. If you have a weakened immune system, it can take five to 10 years.
Cervical cancer is one of the most common cancers in women, and over 270,000 women die each year from the disease. Regular Pap smears are essential for early diagnosis and successful treatment. When the cancer is detected early, it has a high survival rate. HPV vaccination can prevent cervical cancer, although it is not a replacement for Pap smears and cervical cancer screenings.
HPV Vaccination
There are three vaccines that protect against the cancer-causing HPV strains: Gardasil, Gardasil 9, and Cervarix. Gardasil also protects against HPV 6 and 11, which cause most cases of genital warts.
For people aged nine to 14, the vaccines are given in two doses that are six to 12 months apart. For people aged 15 and older, the vaccine is given in three doses. The second shot is administered two months after the first, and the third shot is administered four months after the second.
The vaccines work best when administered before exposure to HPV, so it's ideal to be vaccinated before you become sexually active. The World Health Organization recommends the vaccine for girls aged nine to 13, and the CDC recommends the vaccine for boys and girls aged 11 to 12. You can receive the vaccine up until the age of 26, though.
FAQ
Is the HPV vaccine safe?
The HPV vaccine is perfectly safe for people who are in good health. It doesn't contain a live virus, so it can't cause an HPV infection. Side effects may include headaches, nausea, and dizziness, but these problems are rare and temporary.
If you have a moderate or severe illness, you should wait to be vaccinated until you have recovered. If you have ever had a severe allergic reaction to a component of the HPV vaccine, you shouldn't get the vaccine.
Should I have an HPV test before I'm vaccinated?
The vaccine is recommended regardless of whether or not you have HPV, so a test isn't necessary before getting vaccinated. Although the vaccine won't treat or cure HPV if you already have it, the vaccine can prevent you from contracting another strain of the disease.
What is the likelihood of developing cancer if I have a high-risk form of HPV?
According to a study from the National Cancer Institute, four percent of women who had high-risk HPV developed pre-cancerous cervical disease within three years, and seven percent developed advanced cervical disease within 10 years. People with weakened immune systems from other illnesses are more likely to develop cancer than people with stronger immune systems.
Will HPV affect my fertility or pregnancy?
HPV does not affect fertility, and it isn't linked to miscarriage, premature labor, or any other pregnancy complications. Genital warts rarely cause problems during delivery, but you may need to have a caesarean section if the warts block the birth canal. The disease can be transmitted to a baby during birth, but this is very rare.
If I contract HPV, will I have it forever?
The CDC estimates that 70 to 90 percent of infections are cleared by the immune system. However, researchers aren't sure whether the body entirely eliminates the virus or whether the virus is simply suppressed to such a low level that it can't be detected. Fortunately, even if the body just suppresses the infection, it can't spread to another person in this non-detectable state.
How serious is HPV?
HPV is harmless in most cases, and many people experience no symptoms or complications. However, the high-risk strains of the disease that can lead to cancer should be taken seriously. If you have one of these varieties of HPV, you should visit your doctor regularly for cancer screenings.